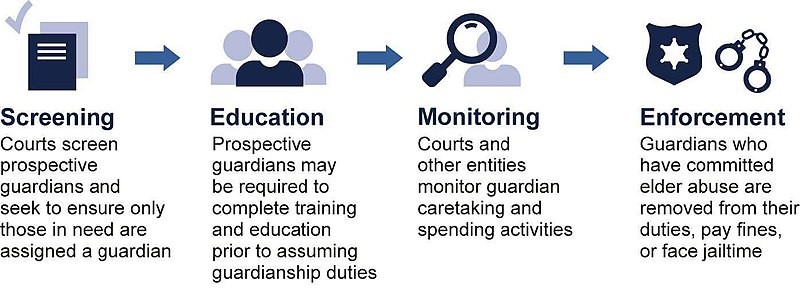
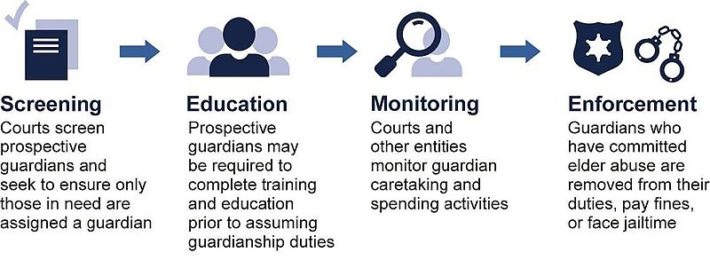
On June 18th this year, Grace Birnstengel a writer/reporter from Minneapolis published an article on Forbes on Elder Abuse, which caught the attention of millions of readers all over the world. The article told a heart wrenching story about how elderly people receives abuse from the very people that are on duty to care for them. The article makes us think, rather re-think the model we have in place for our elderlies and do we need a legal change to make it void of abuse.
Her reports hums a sombre tone which leads our attention back to the ecosystem made by a weird cocktail of healthcare, consumerism, nursing and involuntary abuse (which is not meant to be). And does the current system is a default slope where conditions are going to tumble down to even degraded services and actual abuse of their own clients.
Perhaps the first recorded case in Nursing Home abuses was the New York State Senate Hearing before the Select Committee On Aging House Of Representatives, on February 6th, 1978 New York; Which was about the three yearlong litigation of nursing home profiteer of Bernard Bergman who turned his inheritance of merely $25000 into a gigantic nursing home empire valued $24 Million in 1976. Mr. Bergman was prosecuted by fraud, abuse and mismanagement.

Malnutrition / Dehydration in patients:
The charges on Mr Bergman was concluded by the witnesses who testified to the New York State Senate about patients lapsing into coma due to untreated dehydration, using milk well past it’s expiry date and other mistreatment of the patients.
The snowballing of malnutrition and dehydration in patients can be understood by a quote by an English social reformer Florence Nightingale who said –
“If a patient is cold, if a patient is feverish, if a patient is faint, if he is sick after taking food, if he has a bed-sore, it is generally the fault not of the disease, but of the nursing.”
Malnutrition in patients staying in either private or public nursing homes is prevalent and a default condition. From a study done of 308 elderly resulted in a data which indicated 28.6% of the elderly staying in the nursing home suffered from malnutrition and 44.5% of them were at risk for malnutrition. The problem comes when these patients have to solely rely on nurses and carers to feed them. It could be a test of professionalism and expertise of the nurses who have to care for patients which may show poor appetite, swallowing difficulties, dental issues, and complete eating and drinking assistance.
The malnutrition in patients could be intercepted by early signs of it by BMI check, a basic and humane questionnaire a medical self-assessment.
Although patients with more eating dependency stands as a risk in malnutrition, but these patients can easily be a victim of overworked or simply unfit nurses who cannot provide nursing as an extended and humane professional courtesy.
Bearing this in mind, malnutrition and dehydration in patients can exist with lack of individual care, work load on nurses or simply by negligence.
Malnutrition and dehydration is increasingly prevailing issue with cases and stories which demands attention and an effective solution. With cases appearing globally, it is a cause of alarm.
On May 29, 2020, Pietro Bruccoleri living in a long term care home in Canada succumbed to malnutrition and negligence. His obituary said he was held in the hearts of his family and friends and that he died ‘peacefully’.
It must be hard to imagine writing a modest but final
obituary when after investigation
proved that the death was caused by heavy neglect, malnutrition and a sweltering
hot room. The New Democratic Party of Canada has launched a new independent
public enquiry on the Community Care Home.
Nursing home patient rights
The first need for a legislated Nursing home patient and residents’ rights was
finally noticed in the 70’s when the cases and complaints about patient
mistreatment were pooling and went unheard of in the United States. The 1987
Nursing Home Reform Law was a response to increasing angst about quality care
and negligence in Nursing homes. The reform law promised dignity, privacy and a
quality nursing facility.
But the story of patients’ rights starts with the man who
always spoke his mind: Claude Pepper
Courtly Champion Of America’s Elderly
as The New York Times cites
him in a 1996 article.
Born in 1900 son of a sharecropper Mr. Pepper was long-time advocate of Federal
assistance to the elderly. He became one of the competitor and speaker against
Ronald Regan, when a collections of bills mostly dealing with nutrition, were
spawned. – according
to NY Times.
Mr Pepper was a social reformer who pushed the White House into officially
recognizing the need and demand of a proper legislation which protected the
elderlies in Nursing homes, medical institutions and home care.
“I refuse to believe that a country as rich and powerful as ours can’t afford to guarantee the basic comfort and security of its older citizens. I know we can do it”. – Claude Pepper

With the efforts of the untiring and undefeatable 81 years old Representative Mr Pepper the act of Nursing Home Reforms was added into Budget Reconciliation Act of 1987 under Title IV: Medicare, Medicaid, and Other Health-Related Programs and Subtitle C: Nursing Home Reform.
This 1987 Bill of Rights ensures that each member either a resident or patient in a nursing home is entitled to following rights –
- The right
to live in a caring environment free from abuse, mistreatment and neglect.
- The right
to live without the fear of enduring physical restraint.
- The right
to privacy.
- The right
to receive personal care that accommodates physical, medical, emotional and
social needs.
- The right
to a social contact/interaction with fellow residents and family members.
- The right
to be treated with dignity.
- The right
to exercise self-determination.
- The right
to exercise freedom of speech and communicate freely.
- The right
to participate in the creation and review of one’s individualized care plan.
- The right
to be fully informed in advance of any changes to care plan or status of the
nursing home.
- The right to voice grievances without discrimination or reprisal.
Reporting Nursing Home Abuse
Even though the US has a law supporting its nursing care patients from possible abuses, it’s still hard to ‘catch’ an abuse and even trickier for patients and residents to – report it.
According to WHO nursing home abuse is – “A single, or repeated act, or lack of appropriate action, occurring within any relationship where there is an expectation of trust, which causes harm or distress to an older person.” Most of the elder abuse is generally hidden from public eye either because it goes unreported or the patients or relatives/friends are often reluctant to report the abuse to concerned authorities. It could be because of shame, fear or loss of independence.
“This is likely to be an underestimation, as only 1 in 24 cases of elder abuse is reported” – WHO
The first and foremost way to report an elderly abuse is to care and to observe these signs. Whether it’s the friends and families making frequent visits to the resident or an attentive caregiving staff worker. Once the abuse is recognized, the observer should gather details because often times these abuses could be time sensitive.
He/she can take a picture if there’s a bruise, bedsore or an insensitive action from a staff member. Time and location of the conditions. Proof like this may help a lawyer make a valid and legal case to prosecute for compensation. Some of the patients might have a memory problem or a communication impediment, which hinders the proper reporting.
I saw a nurse hit and yell at the lady across the hall because the nurse told the lady she didn’t have all day to wait on her. The lady made some remark. The nurse hit the lady and said, “Shut up.” – Georgia Nursing Home Resident
To report elderly abuse, a person should immediately contact –
1. The Eldercare Locator, at 1-800-677-1116, during weekdays to find out any specific state information that may apply.
2. Contact the elder’s care physician, immediate family and friends.
3. In life threatening circumstances call 911 immediately.
4. After this, the family may choose to hire an attorney to represent the abuse victim and claim for compensations.